Sustainable Systems

Risk Profiles and Psychosocial Impact of Q Fever
Q Fever is a bacterial infection that spreads to humans from animals particularly cattle and sheep. Not all people who are infected will develop acute clinical symptoms. Those that do, can experience mild to severe flu-like symptoms through to needing to be hospitalized for liver and heart problems. ~15% of those who experience acute symptoms will also develop a chronic fatigue-like syndrome. Many risk factors for Q Fever are known and a vaccine is available.
Identifying the extent to which the community is aware and are at-risk of developing Q Fever is therefore important if we are to reduce the number of incident cases. NEIHR members and colleagues from the Q Fever Research Consortium are currently conducting multiple projects examining awareness and risk profiles among the general population and our agricultural students, who are at high-risk of exposure but are not mandated to be vaccinated. We are also examining the psychosocial impacts of Q Fever among members of our community.
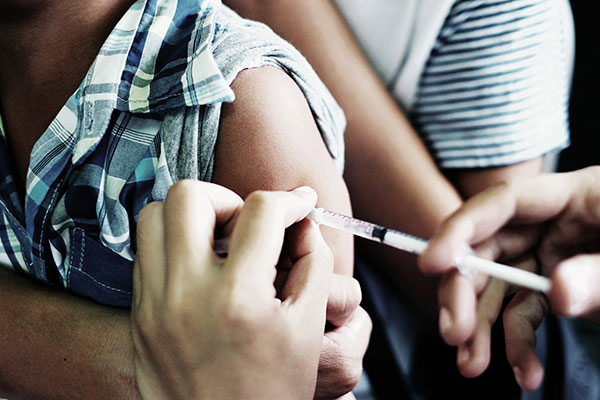
Improving Pre-screening for the Q Fever Vaccine
The current Q Fever vaccine (Q-VAX®) is effective in approximately 80% of people, and is indicated for those at-risk of exposure, aged 15+ years, and for those not previously exposed to the bacteria. Pre-vaccination screening including antibody and skin testing is carried out to determine prior exposure, which can cause severe reactions if subsequently vaccinated.
The Q Fever Research Consortium’s collaborative team is currently developing new pre-screening tools and vaccine preparations that may facilitate vaccination of at-risk populations in Australia.

Successful Refugee Resettlement
Australia receives ~6,000 humanitarian refugees annually with most settling in major cities. Recently, Armidale was announced as the first new humanitarian resettlement location in over a decade. Similar to many regional towns, Armidale has a relatively limited concentration of clinical and education services compared to larger cities.
Given that the humanitarian program is likely to grow into the future and many refugees have high-level or complex needs, NEIHR members, UNE colleagues and collaborators are currently planning a study to examine the availability and effectiveness of existing clinical and language training services in meeting these needs in addition to the needs of the remainder of the community. Community cohesion is also being investigated.

Rural Workforce Capacity
Generalist and specialist healthcare services tend to be concentrated in Australian major cities. This results in significant structural barriers to accessing care including long wait-lists, distance to services and lost productivity costs associated with traveling to appointments. Geographical disparities in care persist, in part, because it is often difficult to recruit quality providers and for these providers to remain in regional and rural areas long-term.
With the object of increasing rural workforce capacity and capability, NEIHR is partnering with clinical stakeholders to strengthen regional and rural recruitment and retainment policies and procedures.

Climate and Our Health
The impact of climate change is felt in human health, from the mental health consequences of drought, concern and stress about the impact of climate change on future generations and the consequences of climate change for disorders and diseases that may become more prevalent or be exacerbated by changes in temperature, air quality and environmental conditions.
With others, members of NEIHR are developing projects that will examine the relationship between weather events and cardiorespiratory mortality rates and the impact of drought and dust on the incidence of Q Fever.

Technology Integrated Health Systems
The limited concentration of clinical providers in regional and rural Australia means that alternate healthcare models are needed to meet the needs of our communities. Significant investment has been made in the development and scalability of technology supported delivery options in the past decade.
NEIHR members are working with healthcare providers to evaluate the relative effects and efficiency of digital health models; and ways in which current practice may benefit from integrating these processes into routine care.


